Doctor fired from ER warns about effect of for-profit firms on U.S. health care

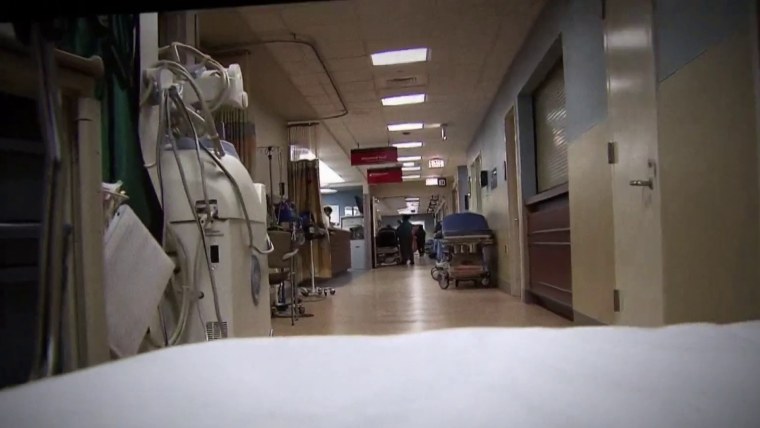
People trying to find crisis therapy at the busy Overland Park Regional Healthcare Centre in Kansas near Kansas Town, Missouri, did not know their basic safety was possibly at possibility. But the professional medical director of the unexpected emergency office noticed the risk in 2012 and for a long time urged his bosses to deal with it by adding staff users.
Then he was fired.
What occurred to the clinical director, a previous Military medical doctor named Ray Brovont, is not an anomaly, some doctors say. It is a developing trouble as far more crisis departments are staffed by for-earnings corporations. A laser concentrate on profits in well being treatment can imperil clients, they say, but when some medical practitioners have questioned the practices, they have been permit go. Physicians who continue to be used see that speaking out can put their careers on the line.
Nowadays, an estimated 40-as well as p.c of the country’s healthcare facility emergency departments are overseen by for-revenue health and fitness care staffing corporations owned by personal equity firms, academic analysis, regulatory filings and internal files clearly show. Two of the largest, according to their websites and information releases, are Imagine Health care, owned by KKR, and TeamHealth, of the Blackstone Group. EmCare, the wellbeing care staffing corporation that managed Brovont, is portion of Visualize.

Non-public fairness companies have taken more than a broad swath of health and fitness treatment entities in the latest a long time. They use significant quantities of financial debt to receive organizations, aiming to enhance their revenue swiftly so they can resell them at gains in a several yrs.
There’s a reason private fairness corporations have invested in corporations staffing medical center unexpected emergency departments, stated Richard M. Scheffler, a professor of health economics and public plan at the University of California, Berkeley.
“The money in the healthcare facility is in the ER,” he reported. “It is the most significant internet generator and a massive revenue center for pretty much all hospitals.” The problem, he stated, is that “ER doctors are currently being instructed how to apply medicine” by financial supervisors.
Brovont, the fired Overland Park unexpected emergency room health practitioner, agreed.
“These directors who make these variations and employ these policies never experience the downstream outcomes of their plan variations,” he mentioned. “They glimpse at the outcome, and the outcome is ‘Hey, we’re earning revenue.’”
3 sites at once
As a former army medical professional who saw overcome in Iraq, Brovont knew how to remedy challenges rapidly. He took that technique to leading the emergency division at Overland Park.
“The target was to discover an difficulty before there was a poor final result,” he said.
1 poor result Brovont hoped to avoid was similar to “code blues,” urgent phone calls to enable Overland Park sufferers whose hearts experienced stopped beating or who were no more time respiration. After the HCA-owned hospital doubled its potential to 343 beds and included a separate pediatric crisis home in 2014, the facility’s code blue plan grew to become unsafe for individuals, Brovont and his 18 fellow ER medical doctors concluded. It needed an crisis department health practitioner to show up at to code blues elsewhere in the medical center, which intended leaving the crisis room without the need of a doctor.
“My medical professionals ended up becoming asked to be in three locations at once,” Brovont reported.
Staffing concerns had been a problem for Brovont considering the fact that he joined the healthcare facility in 2012. He experienced spoken up about them early on, according to files in a lawsuit he submitted alleging wrongful discharge, but acquired nowhere. The enlargement of the healthcare facility designed the issue even worse and introduced the make any difference to a head.

Staffing at the healthcare facility was dealt with by EmCare, a health and fitness treatment staffing corporation owned because 2011 by the private fairness business Clayton, Dubilier & Rice. The agency exited its investment in EmCare in March 2015 after the business issued stock to the general public, but EmCare directors affiliated with Clayton, Dubilier & Rice remained on EmCare’s board into 2017. EmCare grew to become Envision Healthcare and was purchased by a different personal equity enterprise, KKR, in 2018.
In 2015 and 2016, disappointed by the inaction on the code blue policy, Brovont took his and his colleagues’ worries to Dr. Patrick McHugh, his superior at EmCare. Federal legislation expected Stage II trauma facilities like Overland Park to make a physician accessible 24/7 in the crisis section to examine incoming sufferers, Brovont explained to McHugh.
Selecting an additional health care provider would solve the trouble, but that didn’t take place. McHugh acknowledged to Brovont that the choice was monetarily motivated, court information show, and explained in an e-mail to the doctors: “Profits are in everyone’s ideal desire.”
Continuing to argue for a transform in the policy, Brovont sent a memo to management outlining his unit’s fears he was fired six weeks afterwards, in January 2017. “There is a obligation as the company agent to help the corporation’s targets,” McHugh instructed him, according to court docket filings.
In addition, Brovont was barred from working at nearby hospitals whose emergency departments EmCare oversaw. For the reason that he was an unbiased contractor for EmCare and not an staff of the clinic, there was no tribunal to which he could petition against his dismissal.
Brovont, who hasn’t spoken out about his circumstance until finally now, sued EmCare for “wrongful discharge in violation of public policy” in 2017. A jury awarded him $29 million, such as $20 million in punitive damages, which was diminished to $26 million on appeal. That ruling was remaining.
A spokeswoman for Imagine, EmCare’s parent, said in a statement that the firm complies “with condition legislation and operates with substantial ethical expectations that put patients’ well being and protection very first.”
“Envision clinicians, like all clinicians, exercising their impartial judgment to provide good quality, compassionate, clinically suitable treatment centered on their patients’ unique needs,” it explained. “The concern elevated by Dr. Brovont was relevant to a healthcare facility policy, not an Visualize plan, and predates Envision’s current leadership staff.”
McHugh didn’t react to an email and a cellular phone information in search of comment. He no for a longer time performs for EmCare. Overland Park Health care Middle was not a bash to Brovont’s litigation. Clayton, Dubilier & Rice did not answer to a ask for for comment.

Not only does Brovont’s situation shed light on pressures unexpected emergency physicians experience when they are directed by earnings-oriented companies it also illustrates how for-income wellness care entities like Imagine run irrespective of legal guidelines created to bar companies from practicing medicine. For example, the appellate courtroom that dominated in Brovont’s favor cited EmCare’s command of healthcare tactics owned, on paper, by doctors, stating that the company “makes a health practitioner the proprietor of these subsidiaries to comply with the laws, which prohibit a publicly traded business from giving clinical solutions.”
Imagine, primarily based in Nashville, Tennessee, says its crisis medicine group companions with more than 540 amenities in 45 states. As the courtroom famous in the Brovont case, the medical professional who owned the EmCare subsidiaries wasn’t involved with its each day procedure.
30-three states have guidelines preventing nonphysicians from influencing scientific conclusions. They call for wellness care to be presented by entities owned by certified practitioners. California, Kansas, New York, Ohio, Pennsylvania and Texas are among the the states with this sort of regulations.
Commencing in the 19th century, states moved to safeguard sufferers with this kind of actions. Legislators recognized that despite the fact that medical professionals swear a duty to put patients’ pursuits very first, when a for-financial gain entity enters the picture, a force for income could get precedence. Laws can also ban cost-splitting arrangements in between clinical practitioners and nonlicensed people today and entities.
But enforcement of the guidelines has been spotty in current many years. And even when conditions are submitted towards entities working towards drugs illegally, penalties can be modest.
In 2015, for case in point, then-New York Lawyer Normal Eric Schneiderman moved towards Aspen Dental Management, a firm furnishing administrative providers to dental workplaces nationwide. Backed by 3 private equity corporations, Aspen contended it wasn’t accomplishing dentistry. But Schneiderman’s investigators observed that Aspen routinely presented incentives or pressured workers customers to boost profits of dental companies and products and solutions in their offices and shared in dentists’ earnings, a immediate violation of New York legislation.
Schneiderman’s settlement with Aspen Dental, on the other hand, was not even a slap on the wrist. With $645 million in once-a-year revenue at the time, Aspen Dental paid only $450,000 to settle the situation. It didn’t acknowledge the allegations and stated it hadn’t designed choices about dental care.
In bringing the Aspen Dental scenario, Schneiderman claimed it demonstrated the perils of corporations’ working towards medication. The risks are even greater in unexpected emergency departments, explained Dr. Robert McNamara, the chairman of crisis medicine at Temple University’s Lewis Katz College of Medicine in Philadelphia and the chief medical officer of the American Academy of Unexpected emergency Medicine Medical professional Group.
“Putting the financial gain motive in concerning the affected individual and the medical professional can guide to untoward penalties in terms of treatment,” McNamara explained. The businesses “choose how lots of clients an hour your medical professional sees. They can direct some of the testing protocols. They can determine no matter if you are viewed by a health care provider or fewer experienced supplier, a physician’s assistant.”
Asked about McNamara’s criticism, the Imagine spokeswoman said the enterprise “follows an working composition that is popular across the health-treatment sector and extensively applied by nonprofit, privately-held and community groups as nicely as hospitals and insurers. Business-extensive lawful challenges to that structure have proved meritless.”
A drive for gains can also final result in inappropriate and highly-priced admissions to hospitals from crisis departments, which was the foundation for a 2017 situation against EmCare. Soon after physicians arrived forward with allegations of Medicare fraud involving EmCare and a healthcare facility chain that experienced employed it, the Justice Department filed civil satisfies from both entities. EmCare experienced admitted Medicare clients unnecessarily to the hospitals whose emergency departments it oversaw, prosecutors claimed, and received remuneration from the healthcare facility chain for undertaking so. Medicare pays at least three situations additional for inpatient admissions than it does for treatment billed as observation or crisis room visits.
Devoid of admitting the allegations, EmCare agreed to pay $29.8 million in December 2017 to settle the Justice Department’s scenario. (The clinic chain settled with prosecutors later, paying out $260 million without admitting the allegations.) When EmCare settled, Imagine, its father or mother, entered into a company integrity agreement with the Office of Wellness and Human Providers. As is usual below this sort of a offer, the HHS inspector basic agreed not to look for to exclude Imagine from collaborating in Medicare or other federal health and fitness treatment applications if it transformed its practices.
Envision fully commited to “full compliance with all Federal wellness care plan requirements” and developed a compliance software with instruction on anti-kickback measures. Envision’s corporate integrity settlement expires in December.
300 techniques in 20 states
How do personal equity-backed for-revenue well being care corporations like Imagine work in states barring organizations from working towards drugs? Dr. Gregory J. Byrne, an unexpected emergency medicine practitioner in Southlake, Texas, provides a clue.
In modern yrs, Byrne, 70, has been the owner of up to 300 unexpected emergency drugs practices tied to Imagine or EmCare in an array of states, a lawful filing in the Brovont situation reveals. Byrne experienced been employed and compensated by EmCare to be the operator, on paper, of the health practitioner apply operating the unexpected emergency department that Brovont directed at Overland Park.
Until eventually Brovont sued for wrongful termination, however, he said he experienced neither met nor read of Byrne. Primarily based on depositions and testimony in the scenario, Byrne performed no role in the department’s oversight, court docket documents show. McHugh, the EmCare govt, did.
The Missouri appeals judges who ruled with Brovont in his scenario observed that Byrne had owned hundreds of other EmCare subsidiaries in at the very least 20 states.
“The actual range of EmCare subsidiaries he owns alterations each individual month,” the ruling said, “and he does not keep keep track of of them or acquire any management function in any of them. The range does not matter to him mainly because all the revenue of the subsidiaries move to EmCare.”
The judges went on to publish that EmCare compensated Byrne a salary and that it would forward “operational paperwork for the doctor ‘owner’ of the subsidiary to indication.” Byrne, a graduate of the College of Mississippi health care university, is a past president of the Texas School of Emergency Doctors in Austin.
Attained by cellphone, Byrne said: “EmCare is a practice administration corporation. We do not control clinical care — that is a medical professional accountability.” He declined to remark further.
Latest company information display Byrne is listed as an operator at an array of medical doctor practices in 10 states: California, Kansas, Louisiana, Massachusetts, Missouri, New Mexico, Ohio, Oklahoma, Pennsylvania and Texas. Most of the methods have addresses in popular with Imagine. 7 of the states in which Byrne reveals up as possessing or controlling a physician follow have guidelines barring the corporate exercise of drugs. Byrne declined to say how numerous techniques he oversees.
Now, Brovont methods crisis medicine at a clinic close to Overland Park and operates a clinic exactly where he delivers substitute treatment solutions for sufferers with melancholy and submit-traumatic anxiety ailment.
Asked no matter whether Overland Park Regional Health care Centre experienced improved its code blue policy, a spokeswoman explained, “The clinic gives medical professional protection of its pediatric and major unexpected emergency departments at all situations, and our crisis room medical professionals do not leave the E.D. to cover code blues in the medical center.”